Healthcare attorney Zach Simpson goes over what to look for and pay attention to before offering a Groupon for chiropractic services.
Continue readingPatient Brokering & Money Laundering: Bieda Arrests Raise Serious Issues
 Three family members involved in owning an addiction treatment center and/or a toxicology lab were charged in July with patient brokering and money laundering in an alleged scheme involving roughly $2 Million. The allegations arise out of a complex corporate enterprise involving at least four companies and some common ownership between the treatment center and lab. While it’s premature to assume that the defendants did anything illegal, there are some interesting things in this case:
Three family members involved in owning an addiction treatment center and/or a toxicology lab were charged in July with patient brokering and money laundering in an alleged scheme involving roughly $2 Million. The allegations arise out of a complex corporate enterprise involving at least four companies and some common ownership between the treatment center and lab. While it’s premature to assume that the defendants did anything illegal, there are some interesting things in this case:
Complexity Invites Suspicion. Every business owner in the addiction treatment and toxicology lab space knows three things: (1) it’s extremely regulated, (2) law enforcement has an especially sharpened focus on these industries, and (3) insurance companies are very suspect of any situation involving either industry, especially when there is any common ownership. So why then would one construct an enterprise that even “looks” complex or tricky? It intensifies suspicion in an already highly scrutinized business space. This is clearly one of the points of focus in this case. There’s an old saying woven into the mind of every experienced healthcare lawyer: if something can’t be done directly, it can’t be done indirectly. Time will tell if anything in this case was wrong or if there are any good reasons for the corporate structure, but the complexity of the corporate structure certainly invites suspicion. Continue reading
The Debate Over Physician Owned Hospitals
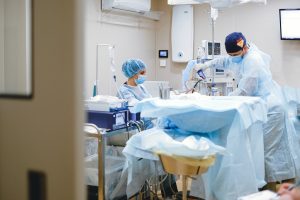 By: Dave Davidson
By: Dave Davidson
The debate over the pro’s and con’s of physician-owned hospitals has been raging for decades. Physician-owners say their hospitals are more patient-focused, provide higher quality care, obtain better outcomes and therefore receive higher patient satisfaction scores. They also point out their convenience and efficiency.
Opponents argue that physician-ownership leads to overutilization and cherry-picking of only the best patients. The less-desirable patients (both clinically and financially) are then left to be taken care of by the community hospitals. For those reasons, both the American Hospital Association and the Federation of American Hospitals remain strongly opposed to physician-owned hospitals.
Federally, the Stark Law includes an exception which allows a physician to refer patients to a hospital in which the physician has an ownership interest, so long as the ownership interest is in the entire hospital, and not just a subdivision of the hospital. However, in 2010, the federal government weighed in again on the issue, and passed the Affordable Care Act (ACA), which includes provisions which (i) restrict physician referrals to hospitals in which they hold an ownership interest; (ii) restrict any increases in physician-ownership of a hospital; and (iii) restrict expansion of physician-owned hospital facilities. CMS has granted exceptions to these restrictions, but those have been limited to rural hospitals and high Medicaid hospitals, and attempts to amend the law have failed.Continue reading
Physician Owned Hospitals Looming Large in Florida
 By: Jeff Cohen
By: Jeff Cohen
Florida may become the “next Texas” on the issue of physician owned specialty hospitals. “Next Texas,” since there are a number of examples where the concept launched (and also flopped). Done right, such facilities could be a better fit for many patients, depending of course on patient co morbidity issues. In theory, they would be the perfect bridge between surgery centers and regular acute care hospitals. But the ability of such specialty focused care suggests a better staffing model and more targeted and efficient overhead, instead of the broad-based overhead of an acute care hospital at is spread out aver all cases, including those where overhead allocation is viewed as “just an expense.” Continue reading
Two Big Changes to Florida’s Patient Brokering Act Affect All Healthcare Facilities and Providers
 Has your attorney ever told you to do your best to comply with certain safe harbors to the Federal Anti-Kickback Statute, and you’ll be likely to survive scrutiny under the Florida Patient Brokering Act (the PBA)? If you’ve heard that, it’s time to re-examine that relationship. In the last month, the Patient Brokering Act has been amended, and then interpreted by a court of law in a way that affects all healthcare providers.
Has your attorney ever told you to do your best to comply with certain safe harbors to the Federal Anti-Kickback Statute, and you’ll be likely to survive scrutiny under the Florida Patient Brokering Act (the PBA)? If you’ve heard that, it’s time to re-examine that relationship. In the last month, the Patient Brokering Act has been amended, and then interpreted by a court of law in a way that affects all healthcare providers.
The Patient Brokering Act has been used in recent years to prosecute abuses in the addiction treatment industry. Other healthcare providers subject to the act have largely been uninvolved in these prosecutions. However, the PBA has been remolded 4 times in the past 5 years as a means to tailor it to allow for prosecutions of bad actors in healthcare, including addiction treatment. One item should be made clear: the PBA applies to any facility at all that is licensed by the Agency for Healthcare Administration (AHCA) or practitioner licensed by the Department of Health (DOH), including physicians, surgery centers, home health agencies, skilled nursing facilities, hospitals, DME providers, diagnostic imaging facilities, clinical laboratories, pharmacies and many other. During the legislative process, barely any healthcare industry representatives (from any provider group) showed up to any legislative workshops or produced counterbalancing input or language proposals that reflected a broader perspective.Continue reading
EKRA and SUPPORT Act Impact: Legal Breakdown
By: Susan St. John
Most everyone knows that laws are being implementing in federal and state government to address the opioid crisis in the US. One such law is the Substance Use Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities Act (“SUPPORT Act”) signed into law in October 2018 by President Trump. While the SUPPORT Act seeks to increase access to treatment for substance use disorders and prevention of substance use disorders, it also contains language to prevent abuse of the process to increase treatment access. Specifically, incorporated into the SUPPORT Act is the Eliminating Kickbacks in Recovery Act (“EKRA”) which directly targets unlawful referrals to recovery homes, clinical treatment facilities, and laboratories.
EKRA is similar to prohibited kickbacks and patient brokering pursuant to Sections 456.054 and 817.505, Florida Statutes, using similar language as both Florida statutes. EKRA makes it unlawful…Continue reading
EKRA Affects Marketing Relationships with Labs and Addiction Treatment Businesses
By: Jeff Cohen
For those following the federal legislative developments on the issue of compensating marketing people who market the services of labs and addiction treatment facilities there is a new update to take note of. Congress passed on October 24, 2018 the “Substance Use-Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities Act.” Yes, that’s a real name! Part of the law is the Eliminating Kickbacks in Recovery Act of 2018 (“EKRA”).
The core aspect of EKRA has to do with how to properly compensate marketing personnel who market the services of labs, addiction treatment facilities and recovery homes. For those of you already familiar with existing federal law pertaining to compensation arrangements (e.g. the bona fide employee exception (the “BFE”) and the personal services arrangement and management contract safe harbor (the “PSA”)), the EKRA provisions will look familiar! Key aspects of this law (which has to be read together with similar existing laws) include—Continue reading
Marketing for DME & Pharmacy Providers: Know Your Subcontractor!
Regulatory compliance is a mandatory investment for any healthcare business owner looking to stay out of serious and personal legal peril, let alone one hoping to keep their company viable.
Yet there is seemingly an onslaught of providers that blatantly run afoul of many of these regulations, knowingly or not, or those that believe they may have found a loophole.
Concerning the latter, there is an important mantra that such DME and pharmacy providers should remember and live by: “[W]hat a provider cannot do directly, it cannot do indirectly through an intermediary.”
Marketing for DME – What exactly am I talking about?
DME providers enrolled with CMS (should) know they cannot solicit or ‘cold call’ Medicare Part B beneficiaries, per the Federal Anti-Solicitation Statute, and that they cannot offer anything of value to a potential patient that could induce them to utilize them as a provider, in accordance with the Beneficiary Inducement Statute.Continue reading
Pharmacy Billing Basics: Know Your Payor!
In giving consideration to whether healthcare regulations apply to a proposed course of conduct it’s absolutely vital for a pharmacy to know its payor! This is especially so in the context of patient marketing and the various regulatory prohibitions on paying for healthcare referrals. Unfortunately, some pharmacy owners remain a bit mixed up about who the ultimate payor is for the medications they dispense, and, depending on that pharmacy’s billing operations, such mistakes can have devastating consequences.
A large part of this confusion might be attributed to the fact that in most instances, a pharmacy is not billing the ultimate payor directly (unlike a DMEPOS provider that may be directly submitting claims to Medicare Part B), but rather, the pharmacy is billing an intermediary entity called a Pharmacy Benefit Manager (“PBM”), which is usually a commercially run entity (non-government owned) that manages and adjudicates claims on behalf of health insurance plans that cover pharmacy benefits.Continue reading
State Patient Brokering Act Cases to Throw out Legal Advice as Defense
 By: Jeff Cohen
By: Jeff Cohen
There are two criminal cases pending in Palm Beach County that threaten to put a bullet in the heart of healthcare professionals and businesses and also the law practices that advise them. Both State v. Simeone and State v. Kigar have a motion from the State pending before them to block any testimony that the defendants received legal advice concerning a contract entered into by an addiction treatment facility and a sober home. The State alleges that the contract violates the state Patient Brokering Act (PBA) because it was essentially a ruse whereby the addiction treatment facility was just paying for the sober home to refer patients. Now the State wants to make sure that the entire issue of the defendants being advised by counsel never sees the light of day.
How is this possible? How can it be that a client can seek legal counsel, get advise (and presumably follow it), and then be blocked from presenting that evidence? The State argues that the PBA has no wording that requires them to prove intent. And if intent isn’t an element to be proven, the argument goes, then evidence of the client intending not to violate the law by getting advice beforehand is inadmissible! Continue reading



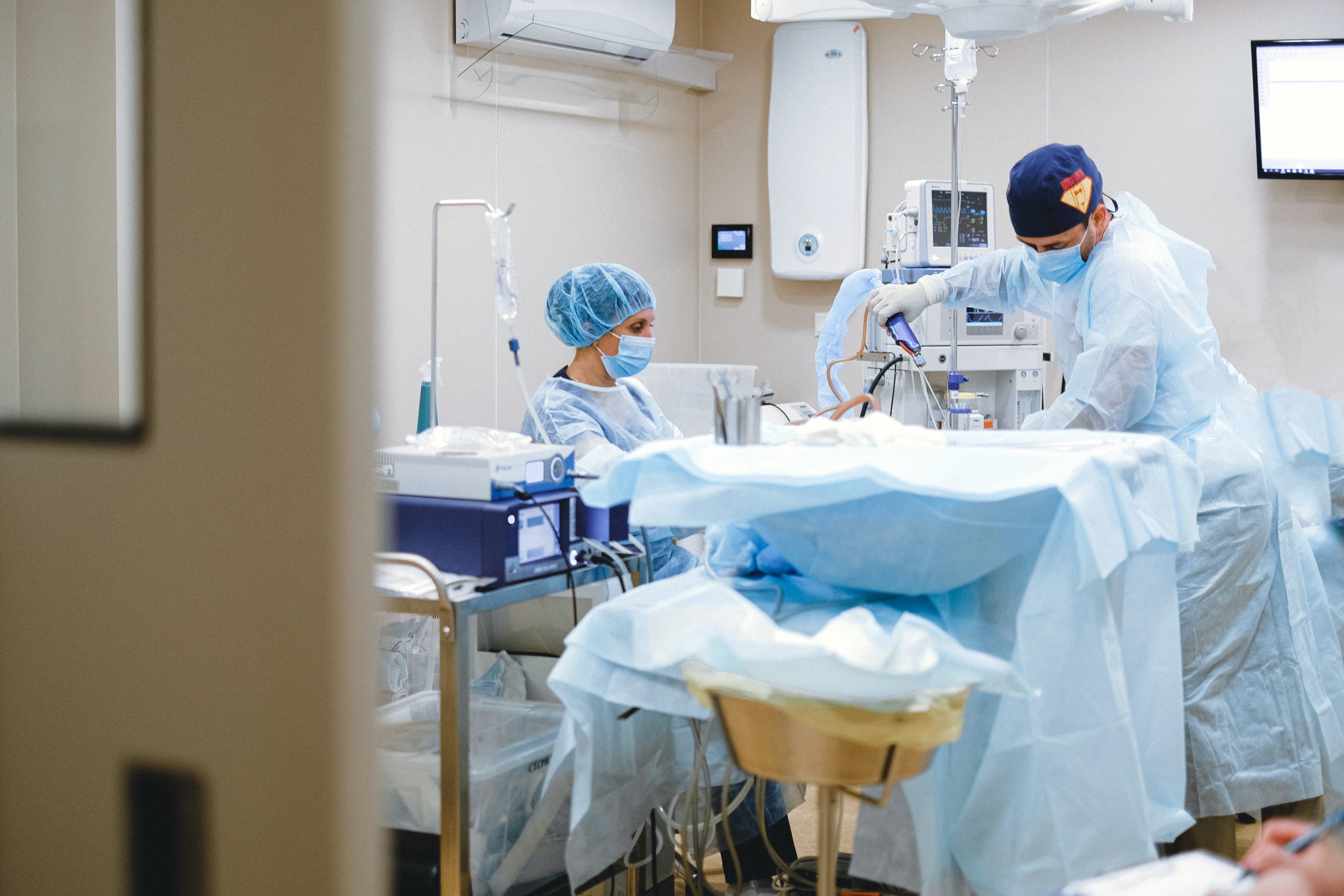



 By:
By: